Some of the hardest times for feeding a newborn begin while in the hospital. Our breasts do not feel full, baby is super sleepy and not always waking frequently to eat. OR baby is constantly eating for periods of time. Naturally we wonder, “Is baby getting enough?” Even if parents keenly listen for swallows, they can still be unsure if the baby is getting enough, as audible swallowing isn’t always consistent during the colostrum phase.
The Golden Hour
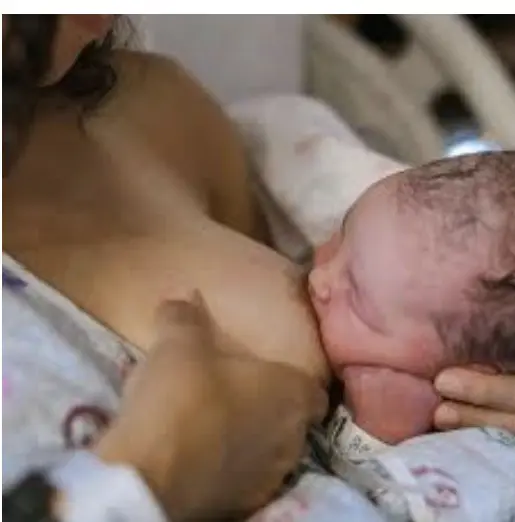
Baby is born, placed skin to skin for “The Golden Hour,” and allowed to breastfeed when showing cues to latch. Baby latches, nurses for a bit and then sleeps. And sleeps. And sleeps.
We know the “birthday nap” within the first 24 hours post-birth is normal for a newborn, but it remains stressful for a parent unable to measure their baby’s milk intake. So how CAN we know baby is getting what they need?
Lactogenesis I
First let’s talk about lactogenesis, or the production of milk. Lactogenesis I typically begins around 16 weeks of pregnancy. Colostrum begins to be made. Some moms may experience leaking of colostrum and some none at all. Whether you leak colostrum or not has no bearing on future milk production.
Colostrum is the first milk made for those beginning feeds following birth. It provides essential nutrients and acts as a post-birth laxative to clear the baby’s meconium. Up to two-thirds of the cells in colostrum are white blood cells that guard against infections, as well as helping your baby start fighting infections for themselves.
Though smaller and thicker than later milk, it’s packed with essential nutrients like protein, vitamins, and minerals for the baby. Their stomachs are also very small initially, about the size of a cherry, so it does not take much to fill that space. The fact that colostrum is less in volume not only correlates well with a tiny tummy, it also is the perfect practice time for baby to learn how to coordinate suck-swallow-breathe patterns required for feeding. These slower flow, lower volume feeds help them become gradually acclimated to the larger volume, greater flow of milk to come.
Lactogenesis II
Lactogenesis II, or milk “coming in” or “coming down” begins for most mothers between day 3 and 5 postpartum. The volume begins to gradually increase over the following days and mom will typically feel breasts feeling heavier, and looking fuller and often will more easily hear baby swallowing during feeds. In conjunction with this increased volume of milk, we see baby’s stools changing from the sticky black meconium to a thinner consistency, dark greenish stool and then onto traditional yellow, seedy stools which is typical for a breastfed baby. Variations occur if baby is also taking any formula during this time.
Latch
Ideally you get baby latched comfortably with a wide-open mouth, or gape, at the breast. This means baby does not just have the nipple in their mouth, and they also are not slurping the breast into their mouth. Baby is opening wide, as if yawning, and the breast tissue is filling their mouth as they close. Think of how you eat a big burger. You open your mouth wide; you lay the bottom part of burger into your lower jaw and then sandwich the rest of the burger in before you bite down. This is how we want the breast to go into baby’s mouth!
Satiety
Outside of watching and listening for swallows, you then observe baby behavior after coming off breast. Does baby seem content? Milk drunk as it is often referred to. Or do they still root and seem hungry?
Output

In addition to working on latch and observing satiety following feeds, you will watch diaper output. The first day of life we expect baby to have 1 dirty and 1 wet diaper. Day 2, 2 dirty and 2 wet and so on through Day of life 4. Usually by this time mom’s milk has begun to increase so baby will be having several wets and several dirty diapers each day.
Weight
Hospital staff weigh the baby after birth and then weigh the baby each day thereafter. Babies typically lose weight after birth, but ideally, they should not lose more than 10% of their birth weight before leaving the hospital. Weight loss is commonly 7% to 8% of birth weight or greater by the third day after birth among healthy, full-term, breastfed newborns. Several factors such as induction, scheduled or emergency c-sections, and prolonged labor with intravenous fluids can impact the baby’s weight at birth. If mom has IV fluids, this can impact and inflate baby’s birth weight, which can increase the percentage of weight loss for newborn.
First 24 Hours
- Latch baby within first hour following delivery
- Skin to skin as much as possible, dad can and SHOULD do this too!
- Unwrap the baby if they’ve been sleeping for more than a few hours; sometimes, just doing so helps them realize they’re ready to eat! Babies eat reflexively, so being swaddled up can hinder those reflexes from firing.
- They will likely take that birthday nap! Most babies who do this will sleep for 6-7 hours despite feeding attempts. Hospital staff can check blood glucose with a simple heel prick while the baby is skin-to-skin with mom if there are concerns. The result will guide the next steps.
- Hand expression will be your best friend if you are trying to avoid supplementing!
The Next 24 Hours: Baby’s Second Night
Whereas baby was snoozing away yesterday, today baby is ready to “party all the time.” Can you hear the song I am thinking of? https://www.youtube.com/watch?v=iWa-6g-TbgI Hey, sometimes we have to laugh or we will cry. SO this is a time to take that approach. Baby is instinctually wanting to eat nonstop and fuss anytime they don’t have the breast in their mouth so you put them back on the breast. By doing this, they are telling your body “Bring it On!”
Let Us Help You
The hospital time with your newborn, especially your first time, brings so many new experiences, new roles in your life. Let Bayou City Breastfeeding help you feel confident and prepared with a Prenatal Consult! We will cover everything above and more. For your convenience, we offer virtual, in-home or office lactation visits.
